But…What Are Mammos Actually Looking For?

Every year during October, we paint the world pink. NFL players wear pink cleats, events are held across the country to raise awareness and support for breast cancer patients, their families, and lifesaving research.
Extra! Extra! Get Your Annual Mammogram!
Everyone, always, during October AKA Breast Cancer Awareness Month
But what do you actually know about what your doctor is looking for on a Mammogram?
If you answered, “Signs of breast cancer, duh!” You’re not wrong. But what are those signs and how can they help you better understand the procedure, why it is so important to go ANNUALLY for a mammogram, and what an abnormal result might mean? …And you might be surprised to learn that an abnormal mammogram, while definitely cause for further screening, is usually NOT cancer.
Who actually “reads” or looks at mammograms?
While your Primary Care Provider is integral in getting you an order for a mammogram, they are not generally the ones reading your mammogram results. They leave that to a Radiologist, who has been specially trained in the diagnosis of diseases and conditions using imaging technology, like an x-ray or a mammogram. They communicate their findings to your Primary Care Provider and/or any other members of your care team for further testing or clearance if everything is well.
What are they looking for?
According to the American Cancer Society, “The doctor reading your mammogram will be looking for different types of breast changes, such as small white spots called calcifications, abnormal areas called masses, and other suspicious findings that could be signs of cancer.”
Let’s dive into that a little more in depth so you can understand the difference.
Calcifications
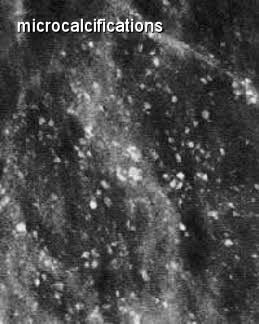
Calcifications are basically calcium deposits in your breasts that may or may not be caused by cancer. These types of spots on a mammogram can be broken down into macrocalcifications and microcalcifications. Of course, macro means they’re bigger and micro means they’re smaller, but in this case, the old adage “Bigger is better,” is true, as macrocalcifications are generally related to aging and do not require further diagnostic testing, whereas microcalcifications, although just mere specks on a mammogram, may need further testing based on how many there are and how they are arranged within the breast tissue.
Masses
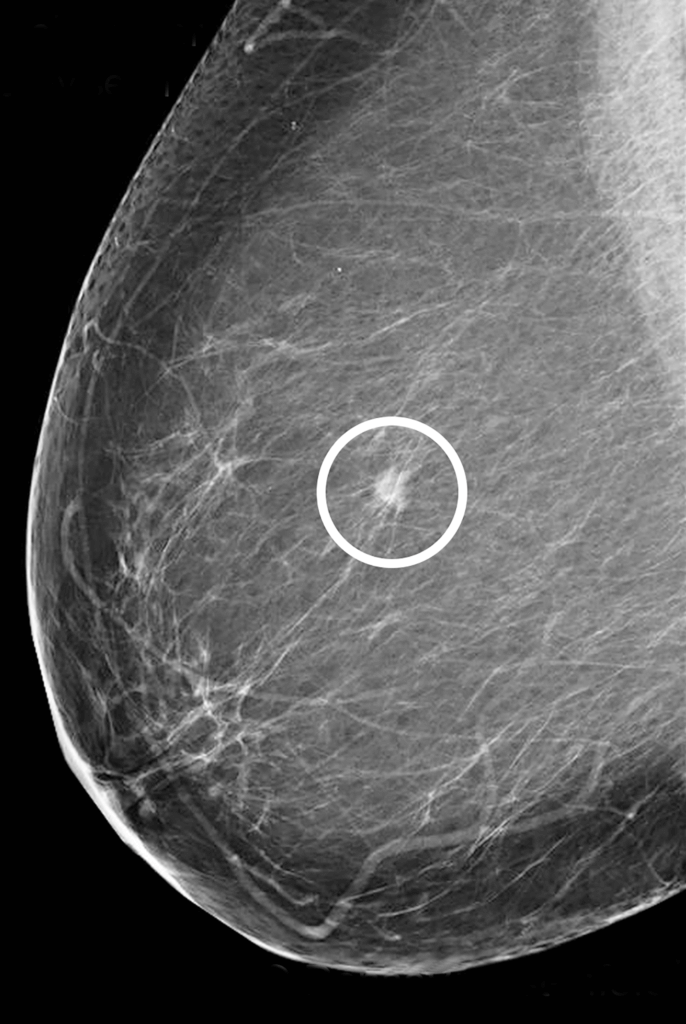
This tends to be what everyone assumes a mammogram is looking for, and that is partly true. Location and identification of any areas that have edges or a shape different from surrounding tissue within the breast can be accomplished using a mammogram, however, there are many types of masses that are no cause for concern, like cysts or non-cancerous solid tumors.
Cysts are fluid-filled sacs and most have thin walls. They are generally not cause for concern and if there is any question, they can be confirmed and drained during a minor procedure.
Solid masses detected on a mammogram tend to be more cause for concern, but there are still many types that are non-cancerous. If a mass is located and isn’t clearly identified as a simple cyst, a breast ultrasound may be ordered as a follow up test, as this technology is better at showing whether something is fluid-filled or solid. A radiologist looks at things like the size, shape, and edges of a mass to determine what it is and if its presence indicates the need for further imaging or diagnostic tests.
Tissue Patterns
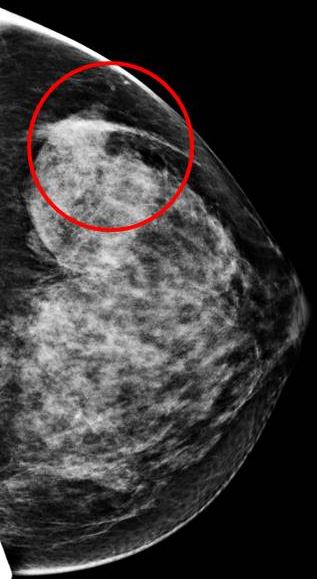
Radiologists also pay attention to places within the breast that have differing tissue patterns, or asymmetries compared to surrounding or normal tissue patterns. These usually show up as white areas within the breast image from a mammogram. Depending on the differences noted, further imaging or diagnostic testing may be needed to assess these asymmetries and their risks.
Distortion or “Pulling”
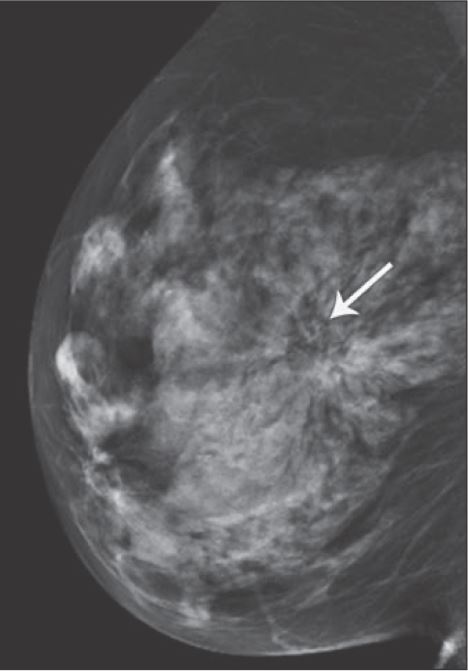
Another thing your radiologist will look for on a mammogram are areas where your breast tissue appears to be “pulling” toward a certain point or distorted. This is referred to as architectural distortion and could be as simple as how the breast was positioned during the mammogram, but also could be a sign of breast cancer, so when this is noted, typically further diagnostic testing is ordered.
Density
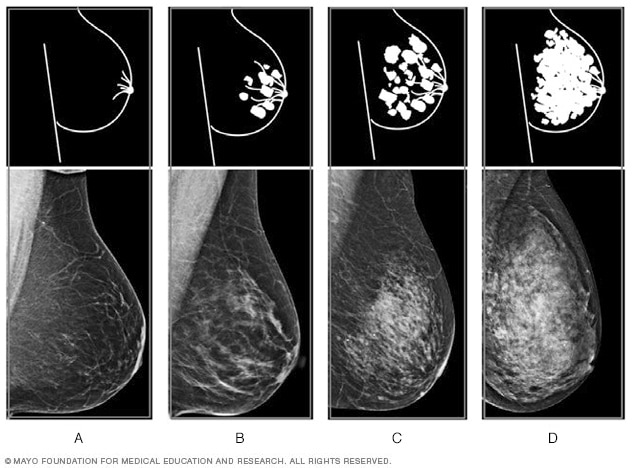
You will receive a breast density reading and risk assessment with your annual mammogram as well. Breast density is simply a measure of how much fibrous and glandular tissue you have in your breasts vs. fat tissue. Studies show that women with more dense breasts have an increased risk of breast cancer and due to the appearance of the more dense tissue on a mammogram, their results can be harder to read. Your risk assessment may indicate that you need more frequent mammograms or additional screenings based on your individual risk factors, including breast density.
Changes Over Time
OK. This one is key. If you haven’t read anything else in this blog, read this.
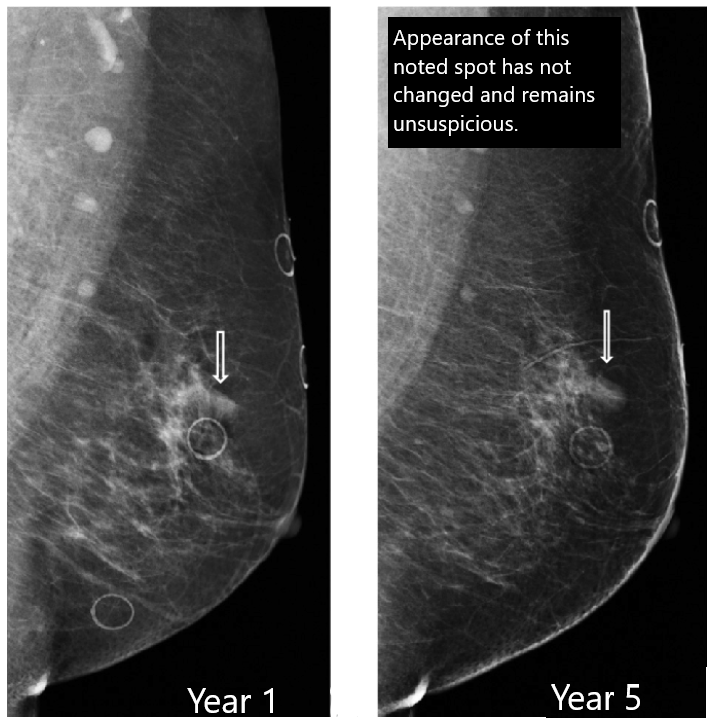
Radiologists use all the available images in your record to help look for any and all of the above breast cancer indicators as well as CHANGES OVER TIME. This means that they will compare your previous images with your current to see if negligible distortion or calcifications have gotten bigger, changed shape, or are starting to cluster in a certain area. Without annual mammogram images to compare, this key component of a strong breast cancer screening plan is lost.
Ensuring that you are going in annually, or more frequently based on your risk factors, ensures that your radiologist can notice new, different, bigger, and more significant patterns in your breast tissue that may end up saving your life.
So, what are you waiting for?
Book your mammogram today by calling 228-809-2355 and make sure to stay up-to-date on screenings, because when you catch it early, you have more options and more hope.
Content inspired by Healthcare is Selfcare: The Podcast.